Analyzing the Clinical Significance of 20/30 Visual Acuity
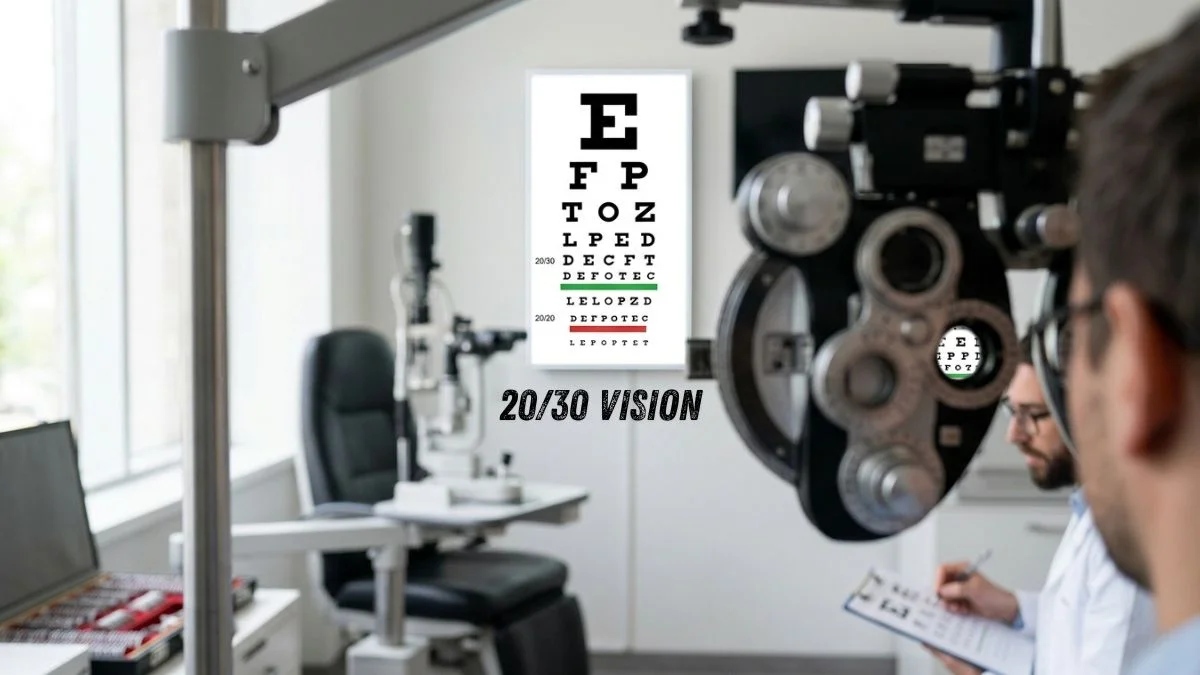
Understanding 20/30 vision starts with defining the mechanics of the Snellen char. The search for this term usually stems from a recent eye examination result. Patients often wonder if this specific measurement necessitates immediate corrective intervention. It represents a visual state where clarity is slightly below the standard baseline. This guide provides the technical clarity required to navigate these optical findings.
When a clinician records 20/30 vision, they describe a specific spatial resolution. The patient sees at 20 feet what a standard eye sees at 30 feet. This indicates a roughly 33 percent decrease in distance visual acuity levels. While not legally blind, it impacts high-detail tasks like reading distant signs. Many individuals function daily without noticing this subtle blur in their environment.
Modern users seek to understand if 20/30 vision is ‘good’ or ‘bad.’ The answer depends entirely on the specific lifestyle and vocational requirements. A commercial pilot requires higher standards than a casual office worker. Consequently, the intent behind the query is often rooted in safety concerns. We must examine the physiological causes to provide a truly comprehensive answer.
The Snellen Framework and International Optometric Standards
The optical industry relies on standardized protocols to measure visual performance. The ISO 8596 standard specifies the requirements for visual acuity testing equipment. This ensures that 20/30 vision measured in London matches 20/30 in Tokyo. Clinicians use these benchmarks to determine the necessity of corrective lenses. Regulatory bodies like the FAA or DMV use these metrics for licensing.
The ANSI Z80.1 Standard for Prescription Integrity
The American National Standards Institute (ANSI) maintains the Z80.1 standard. This protocol dictates the tolerance levels for ophthalmic lens manufacturing. When correcting 20/30 vision, the lens must meet precise dioptric accuracy. Small deviations in manufacturing can result in sub-optimal visual outcomes. Compliance ensures that the prescribed correction effectively moves the patient toward 20/20.
Translating Optical Specifications into Real-World Clarity
Moving from 20/30 to 20/20 vision involves specific refractive adjustments. Corrective features provide significant value across various daily activities. Enhanced contrast sensitivity allows for better performance in low-light conditions. Reducing ocular fatigue is a primary benefit of addressing minor refractive errors. This mapping illustrates why even ‘slight’ correction matters for long-term health.
NOTE: Any surgical intervention or prescription change must be performed by a licensed Doctor of Optometry or Ophthalmology. Self-diagnosis using digital screens may lead to inaccurate results and improper treatment.
Comparative Analysis of Visual Acuity Levels
| Acuity Level | Functional Capability | Common Recommendation |
| 20/20 | Standard Clarity | Routine Monitoring |
| 20/30 | Mild Blur at Distance | Optional Correction |
| 20/40 | DMV Minimum Threshold | Mandatory Correction |
The Roadmap to Correcting 20/30 Vision
Step 1: Comprehensive Eye Examination. Schedule a dilated exam to check health.
Step 2: Refraction Testing. Use a phoropter to find the ideal prescription.
Step 3: Frame and Lens Selection. Choose materials that optimize light transmission.
Step 4: Adaptation Period. Allow the brain 7 to 10 days to adjust.
Step 5: Follow-up Evaluation. Ensure the correction meets the initial visual goals.
Advanced Pathophysiology of Refractive Errors
The human eye acts as a complex biological camera system. Light enters through the cornea and is focused by the crystalline lens. In 20/30 vision, the focal point often falls slightly in front of the retina. This condition is known as myopia, or commonly, nearsightedness. Alternatively, astigmatism can cause light to scatter across multiple focal points. Each anatomical variation requires a specific geometric correction via lenses.
Technological advancements in wavefront aberrometry allow for precise measurements. These systems map the unique ‘fingerprint’ of a patient’s visual system. Higher-order aberrations contribute to the 20/30 measurement in many cases. Traditional glasses focus on sphere and cylinder but ignore these nuances. Modern digital lenses can now address these complex distortions effectively.
The Final Verdict on 20/30 Vision Correction
The conclusion is clear: 20/30 vision is a functional but imperfect state. While it allows for most activities, it represents a loss of peak performance. Corrective measures are highly recommended for those seeking maximum safety. The long-term benefits of ocular comfort outweigh the cost of correction. Therefore, seeking professional consultation remains the definitive winning strategy.
FAQs:
Can 20/30 vision be improved naturally without surgery?
There is no peer-reviewed evidence that eye exercises cure refractive errors. While rest can reduce strain, anatomical issues require physical or surgical correction.
Is 20/30 vision legal for driving without glasses?
In most jurisdictions, 20/40 is the minimum requirement for a standard license. Therefore, 20/30 is usually legal but may cause difficulty at night.
How often should I check my vision if it is 20/30?
An annual exam is recommended to monitor for progression. Significant changes might indicate underlying health issues like diabetes or cataracts.
Does 20/30 vision qualify for LASIK surgery?
Yes, LASIK can often correct 20/30 vision to 20/20 or better. However, a surgeon must evaluate corneal thickness and stability first.
Is 20/30 vision considered a disability?
No, 20/30 vision is not a disability. It is a mild refractive error that is easily managed with standard eyewear or contact lenses.